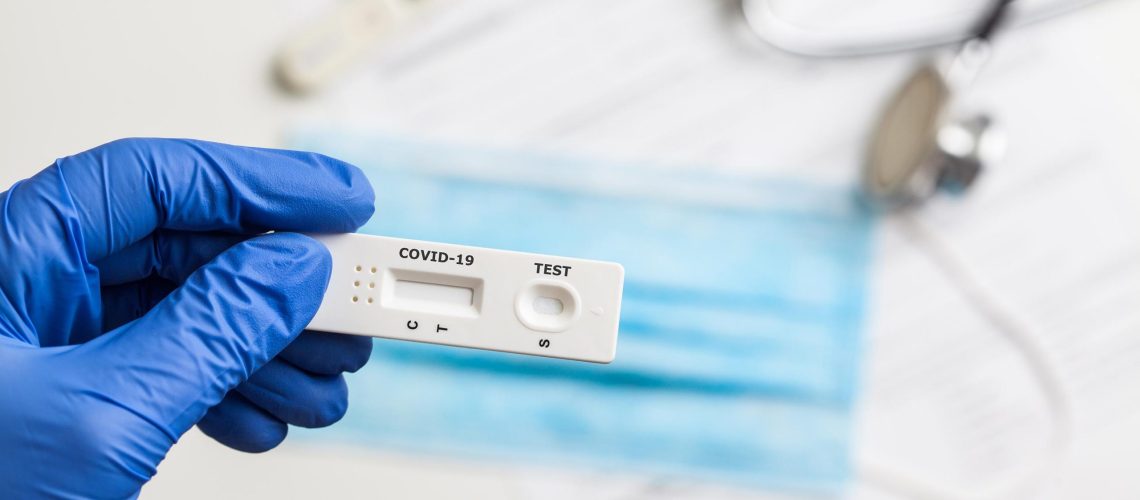
A study performed in Ticino in Spring 2020, on data of SARS-CoV-2 serological tests run on healthcare workers, shows that COVID-19 antibodies are detectable in up to 10% of the participants. Such a result are comparable with the ones of the Corona Immunitas study conducted on the Ticino population. More importantly, it shows that healthcare workers with exposure to COVID-19 patients have only a slightly higher absolute risk of seropositivity than those without, suggesting that the use of protective measures in hospitals aiming at reducing nosocomial viral transmission are effective.
The study was made possible thanks to the collaboration between the EOC, the Institute for Research in Biomedicine (IRB, affiliated to USI), Humabs BioMed (a subsidiary of Vir Biotechnology), USI Institute of Public Health, Clinica Luganese di Moncucco (CLM), Cardiocentro Ticino and Hildebrand clinic. It involved 4,726 healthcare workers from hospitals in the Canton. The study’s goal was to assess whether those involved in the hospital care of COVID-19 cases are presumably exposed to a higher risk of getting the disease than the general population. The results were published recently in the collection Regional Health Europe of the renowned journal Lancet.
The study, carried out between 16 and 30 April 2020, involved healthcare workers with varying COVID-19 exposure risk depending on their job function and working site. The 4,726 employees who gave venous blood samples were also asked to answer specific questions to collect relevant information such as the context (work-related and personal, including any contact with persons who have contracted COVID) and current health conditions in relation to clinical symptoms of infection (further reading on this study).
“The serological test used at the IRB was developed by the Dr. Davide Corti research group at Humabs BioMed and measures antibodies against the portion of the virus responsible for the infection of host cells. Validation experiments have confirmed the specificity and sensitivity of the test,” explains Prof. Federica Sallusto, Laboratory Director at the IRB. “In any case, it is important to remember that the presence of specific antibodies does not yet allow us to determine whether someone is protected, partially or totally, from re-infection. Therefore, it is important to follow up with the participants who have developed antibodies after infection and with those who will develop them after the COVID-19 vaccination. For this, we count on the extraordinary collaboration of the volunteers who joined the study,” says Prof. Sallusto.
Data analysis showed that 69% of participants reported experiencing mild symptoms related to COVID in the two months prior to sampling, 21% did not have any symptoms, while only 7% reported moderate symptoms. “The distribution of participants reporting or not reporting symptoms linked to COVID was similar across risk categories,” – explains Prof. Alessandro Ceschi, Head of the Istituto di Scienze Farmacologiche della Svizzera Italiana and Director of the EOC Clinical Trial Unit, and Professor at the USI Faculty of Biomedical Sciences – “however, the results showed that although there is a slightly higher absolute risk of seroconversion for healthcare workers with direct patient contact, there are no significant differences between hospitals dedicated to the treatment of COVID patients and non-COVID facilities. That leads us to say that working in direct contact with COVID patients with appropriate protective measures is not a risk factor in itself.“
The study result also revealed another interesting aspect: the highest risk of seroconversion is household contacts with proven cases of COVID. The highest seropositivity (19%) was detected in workers exposed to COVID at home; while in others, seropositivity was 8%. “The study conducted with health care workers generally recorded the presence of antibodies in 10% of the participants. The prevalence was only 3% higher in high-risk employees than in the general population of the Corona Immunitas USI-SUPSI-EOC. This result shows the effectiveness of the individual protection measures and the other prevention measures (hand hygiene and social distances) implemented within hospitals” concludes Prof. Ceschi.
Article:
Risk assessment and seroprevalence of SARS-CoV-2 infection in healthcare workers of COVID-19 and non-COVID-19 hospitals in Southern Switzerland
Piccoli, L. Ferrari, P. Piumatti, G. Jovic, S. Fernandez Rodriguez, B. Mele, F. Giacchetto-Sasselli, I. Terrot, T. Silacci-Fregni, C. Cameroni, E. Jaconi, S. Sprugasci, N. Bartha, I. Corti, D. Uguccioni, M. Lanzavecchia, A. Garzoni, C. Giannini, O. Bernasconi, E. Elzi, L. Albanese, E. Sallusto, F. Ceschi, A.
in The Lancet Regional Health – Europe (2020)